|
OADES,
R. D. & DANIELS, R. (1999): Subclinical
polydipsia and polyuria in young patients with schizophrenia or obsessive-compulsive
disorder vs. normal controls. Prog. Neuro-Psychopharmacol. & Biol.
Psychiat. 23, 1329-1344. [request
a pdf copy]
In accord with our understanding of journal policy,
we present the pre-publication
text (view).
The original publication (cited above: doi:10.1016/S0278-5846(99)00069-X)
is available at
http://www.sciencedirect.com/science?_ob=ArticleURL&_udi=B6TBR-4037MH7-
2&_user=10&_coverDate=11%2F30%2F1999&_rdoc=2&_fmt=high&_orig=browse&
_srch=docinfo(%23toc%235149%231999%23999769991%23190110%23FLP%23display%2
3Volume)&_cdi=5149&_sort=d&_docanchor=&_ct=7&_acct=C000050221&_version=1&_u
rlVersion=0&_userid=10&md5=4395aee05095a05c4d0827a3ae0c67c5
Introduction:
Increased water intake and output is more common among psychiatric
patients than in the general population, especially for patients
with schizophrenia. Animal studies suggest that polydipsia
and polyuria derive, in part, from dopamine dysregulation.
Stimulated by these observations this study sought to elucidate relationships
among water homeostasis, monoamine metabolism, and electrolyte excretion
in schizophrenic patients with and without paranoid hallucinatory
symptoms (PH vs. NP), thought to reflect hyper- and hypo-dopaminergic
states respectively, and to compare these with those shown by
patients with obsessive compulsive disorder (OCD).
Methods:
24hr-urine samples for electrolyte, monoamine and metabolite measures
were taken from 14 schizophrenic patients with PH symptoms, 13 with
predominantly nonparanoid (NP) symptoms, 11 OCD patients and 27 healthy
controls (matched for age, weight and creatinine production). Water
intake and serum electrolytes was sampled during 3-4 hours of psychological
testing.
Results:
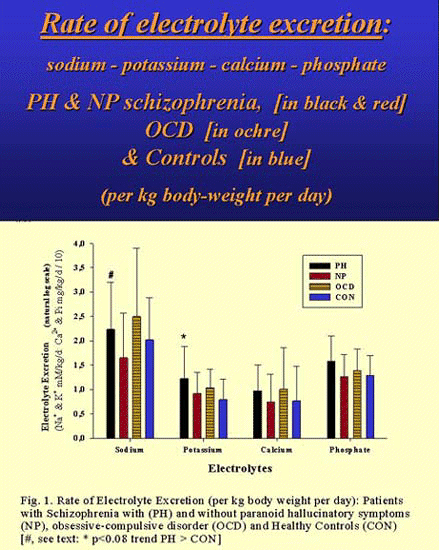 1. PH patients drank 2-3 times
more than the others, yet 24hr-urinary volumes were 75% larger
in both PH and NP patients than in the two comparison groups. 1. PH patients drank 2-3 times
more than the others, yet 24hr-urinary volumes were 75% larger
in both PH and NP patients than in the two comparison groups.
2. Daily potassium excretion was a bit higher in PH patients, but concentrations
of sodium, potassium and phosphate tended to be lower in PH and NP patients
than in the others.
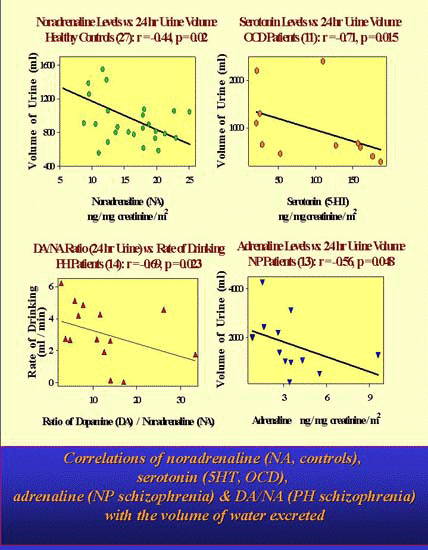 3. Positive associations of
electrolytes with homovanillic acid excretion were consistent across
groups and not directly related to medication. 3. Positive associations of
electrolytes with homovanillic acid excretion were consistent across
groups and not directly related to medication.
4. But associations of electrolyte excretion with noradrenergic activity
in controls were absent in psychotic patients and associations with
serotonin in OCD patients were absent in the other groups.
Conclusions:
Increased water intake and output in PH patients
(i.e. poor water homeostasis) along with the disturbed
association with noradrenergic metabolism (more MHPG excretion)
are consistent with increased autonomic activity in these patients.
The independence of measures of water homeostasis from dopaminergic
medication indicates that the associations in clinically responding
PH patients of polydipsia with DA function (decreased DA levels) may
be pertinent to this subgroup but not to schizophrenia in general.
|


